Diseases & Procedures
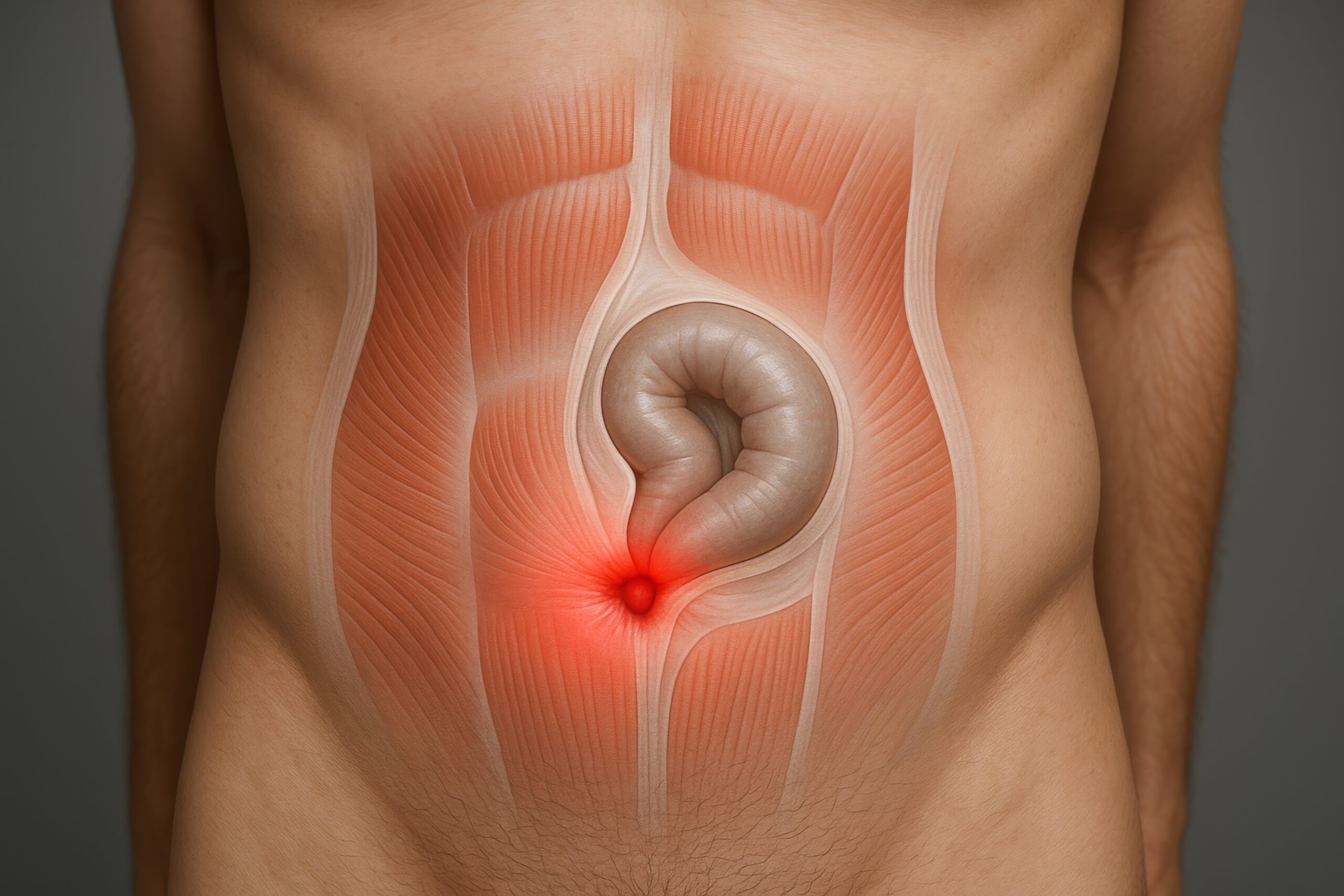
Ventral and Umbilical Hernias
Ventral and umbilical hernias are types of abdominal hernias involving the protrusion of tissue through a weak spot in the abdominal wall muscles and fascia. A ventral hernia can occur at any location on the abdominal wall and may result from previous surgical incisions, making incisional hernias a common type of ventral hernia. An umbilical hernia specifically occurs near the belly button (umbilicus) and is common in infants, though it can also affect adults due to factors such as obesity, pregnancy, or persistent abdominal pressure. Symptoms may include a noticeable bulge, discomfort, or pain, especially when lifting, bending, or coughing. While small, asymptomatic hernias might just require monitoring, larger or symptomatic hernias often need surgical repair to prevent complications like incarceration or strangulation, where the blood supply to the trapped intestinal tissue is cut off. Consultation with a healthcare provider is essential to determine the appropriate management approach based on the hernia’s size, symptoms, and overall health of the patient.
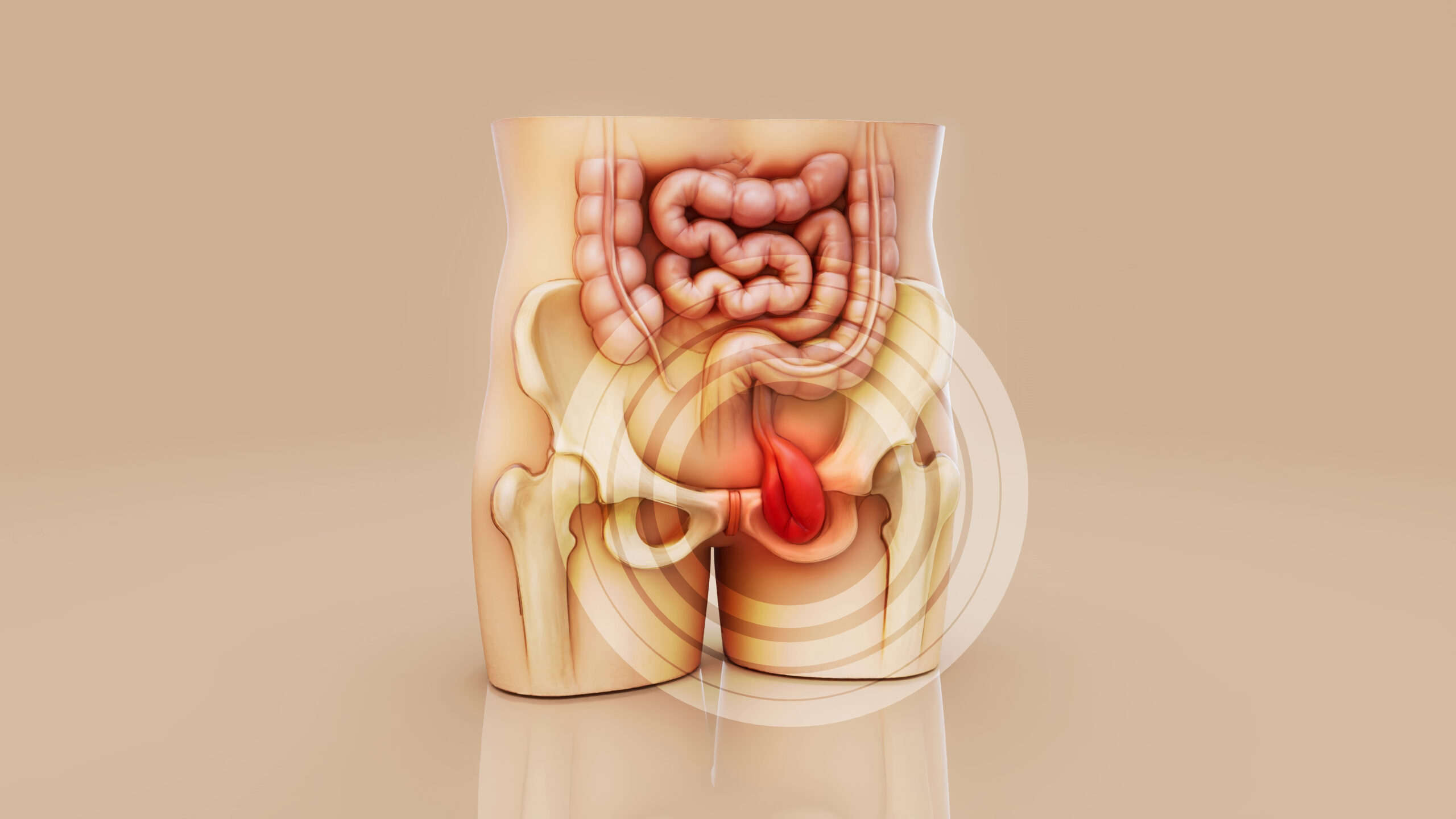
Inguinal and Femoral Hernias
Inguinal and femoral hernias are types of groin hernias that occur when tissue, such as a part of the intestine, protrudes through a weak spot in the abdominal muscles. An inguinal hernia, the most common type, occurs in the inguinal canal, which is located in the lower abdominal wall, and is more prevalent in males. Femoral hernias, less common and more prevalent in females, occur in the femoral canal, which is just below the inguinal ligament and can be more prone to complications such as incarceration or strangulation. Both types can cause a noticeable bulge in the groin area, pain or discomfort especially when bending over or lifting, and in severe cases, lead to obstructed blood flow to the intestines. Treatment usually involves surgical repair to prevent complications and alleviate symptoms, either through open surgery or laparoscopic and robotic techniques. Early consultation with a healthcare provider is recommended to determine the appropriate intervention.

Gallbladder Disease
Gallbladder disease refers to a range of conditions affecting the gallbladder, a small organ located beneath the liver that stores bile, which aids in digestion. The most common gallbladder disorders include gallstones, cholecystitis (inflammation of the gallbladder), and biliary dyskinesia or hyperkinesia. Gallstones can form when there is an imbalance in the substances that make up bile, leading to solid particles that can obstruct the bile ducts. Symptoms of gallbladder disease may include abdominal pain, particularly in the upper right quadrant, nausea, vomiting, indigestion, and jaundice. Diagnosis typically involves imaging studies such as ultrasound or CT scans, as well as blood tests to assess liver function. Treatment options vary depending on the specific condition and severity, ranging from dietary changes to surgical interventions like cholecystectomy, the surgical removal of the gallbladder. Early diagnosis and management are essential to prevent complications associated with gallbladder disease.
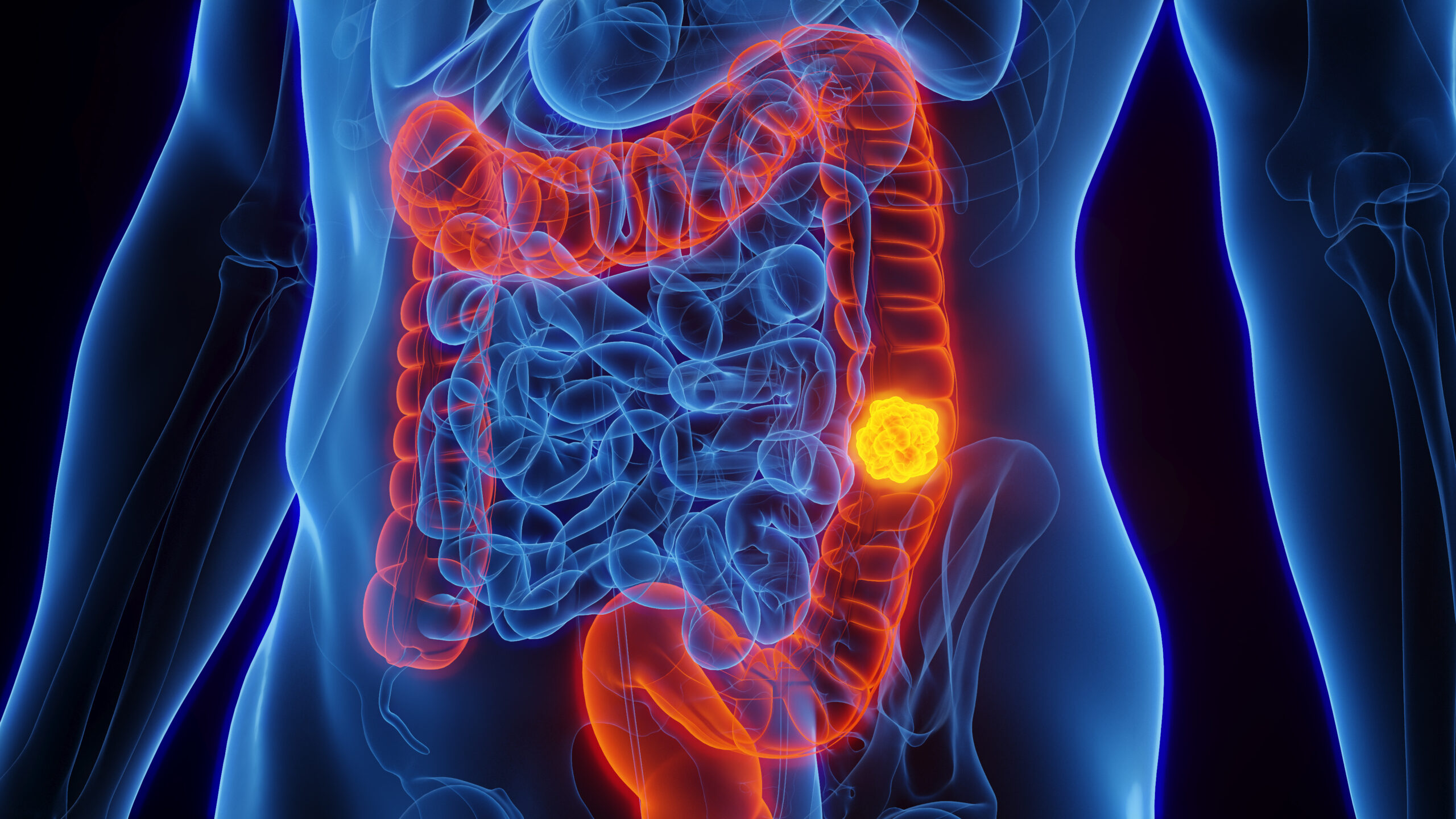
Colorectal Cancer
Colorectal cancer is a type of cancer that occurs in the colon or rectum, parts of the large intestine. Colorecteal cancer is the second leading cause of cancer related death and is becoming more prevalent in younger people. It typically develops from adenomatous polyps, which are benign growths that can become cancerous over time. Risk factors for colorectal cancer include age, family history, certain genetic syndromes, inflammatory bowel diseases, a diet high in red or processed meats, low fiber intake, smoking, and physical inactivity. Symptoms may include changes in bowel habits, rectal bleeding, abdominal discomfort, unexplained weight loss, and fatigue. Diagnosis is achieved through screening methods such as colonoscopy, imaging studies, and biopsy to confirm the presence of cancer. Treatment strategies may include surgery, chemotherapy, radiation therapy, and targeted therapies, depending on the stage and characteristics of the cancer. Regular screening is essential for early detection, which significantly improves treatment outcomes and survival rates.

Colonoscopies
A colonoscopy is a diagnostic medical procedure used to examine the interior of the colon (large intestine) and rectum. During the procedure, a flexible tube with a light and camera, called a colonoscope, is inserted through the rectum and advanced through the colon. This allows the physician to visually inspect the lining of the colon for abnormalities, such as polyps, tumors, inflammatory bowel disease, or signs of colorectal cancer. Prior to the procedure, patients typically undergo bowel preparation to clear the intestinal tract, which may involve dietary changes and taking laxatives. The procedure is usually performed under sedation to ensure comfort. In addition to diagnosis, colonoscopy can be used therapeutically to remove polyps, take biopsies, or treat certain conditions. It is recommended as a routine screening tool for colorectal cancer, particularly for individuals aged 45 and older or those at higher risk. Regular colonoscopies can lead to early detection and prevention of colorectal cancer.
Dysphagia (Difficulty Swallowing)
Dysphagia is a medical term that refers to difficulty swallowing, which can affect the ability to eat, drink, or take medications safely. It may result from a variety of underlying conditions, including neurological disorders (such as stroke or Parkinson’s disease), structural abnormalities (like tumors or strictures), or muscle disorders that impact the swallowing process. Symptoms of dysphagia can include a sensation of food getting stuck in the throat or chest, coughing or choking during eating or drinking, regurgitation, and unexplained weight loss. Diagnosis often involves a thorough medical history, physical examinations, and specialized tests such as a swallowing study (video fluoroscopy) or endoscopy. Treatment depends on the underlying cause and may include dietary modifications, swallowing therapy with a speech-language pathologist, or medical and surgical interventions. Dysphagia can be a symptom of Esophageal cancer and should not be ignored. Managing dysphagia is crucial to prevent complications such as aspiration pneumonia and malnutrition.
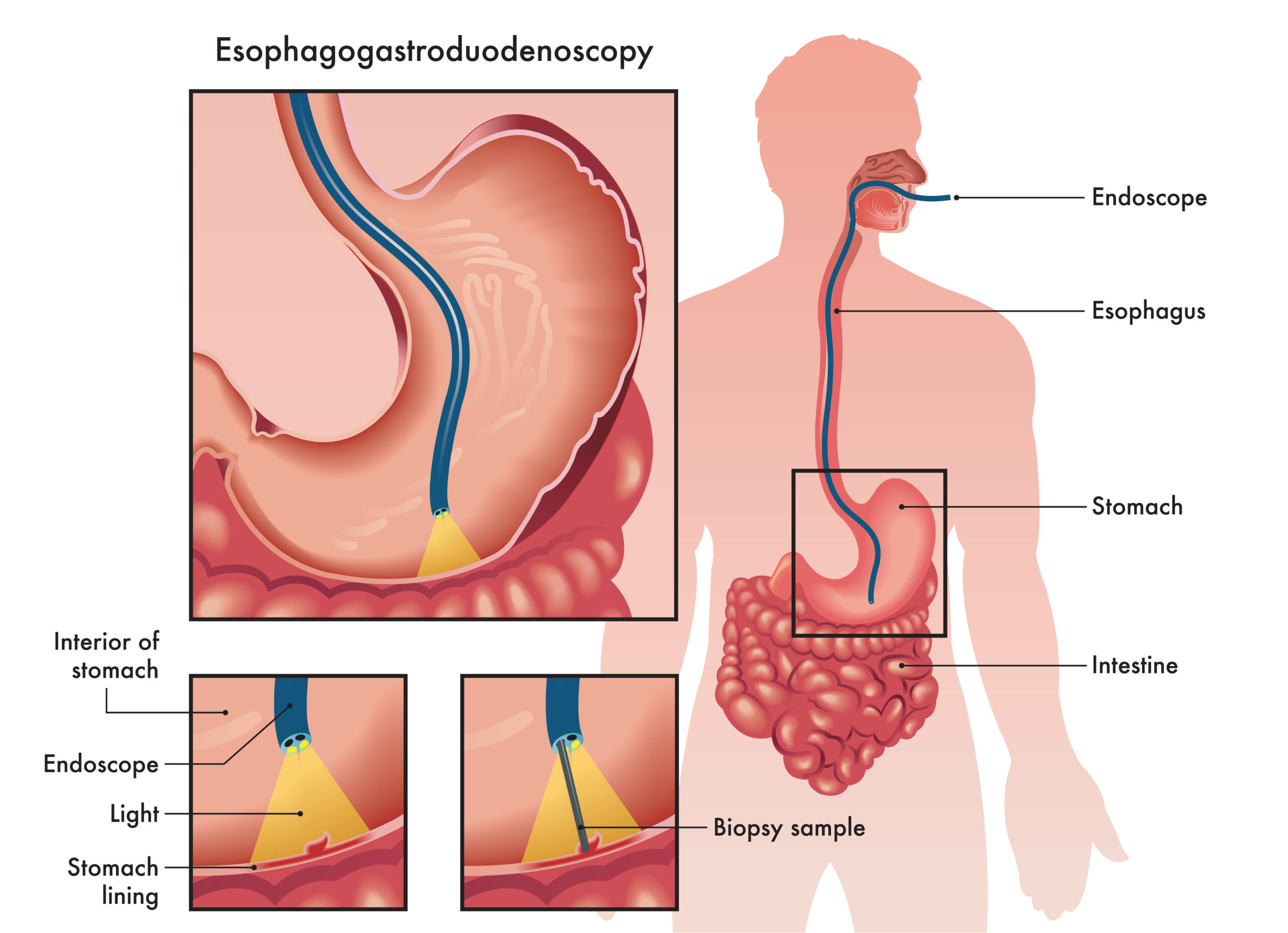
EDG
Esophagogastroduodenoscopy (EGD) is a diagnostic procedure that allows healthcare providers to examine the esophagus, stomach, and the upper part of the small intestine (duodenum) using a flexible tube known as an endoscope. The endoscope is inserted through the mouth and guided down the esophagus, providing a visual assessment of the mucosal lining to identify abnormalities such as inflammation, ulcers, cancerous tumors, or bleeding. The procedure typically requires sedation to ensure patient comfort and may also involve taking biopsies or performing therapeutic interventions, such as removing polyps or treating strictures. EGD is often indicated for patients experiencing symptoms such as difficulty swallowing, persistent abdominal pain, unexplained weight loss, heartburn, nausea, or gastrointestinal bleeding. By enabling direct visualization of the upper digestive tract, EGD is an important tool for diagnosing and managing various gastrointestinal conditions.

Gastroesophageal Reflux Disease
Gastroesophageal reflux disease (GERD) is a chronic digestive condition where stomach acid or sometimes bile flows back into the esophagus, irritating its lining. This backflow, or acid reflux, can lead to symptoms like heartburn, regurgitation of food or sour liquid, chest pain, difficulty swallowing, and the sensation of a lump in the throat. Persistent reflux can result in complications such as esophagitis, Barrett’s esophagus, and an increased risk of esophageal cancer. Factors contributing to GERD include obesity, pregnancy, smoking, certain foods and medications, and a hiatal hernia. Treatment typically involves lifestyle changes, dietary adjustments, medications, and in some cases, surgery to manage symptoms and prevent complications.
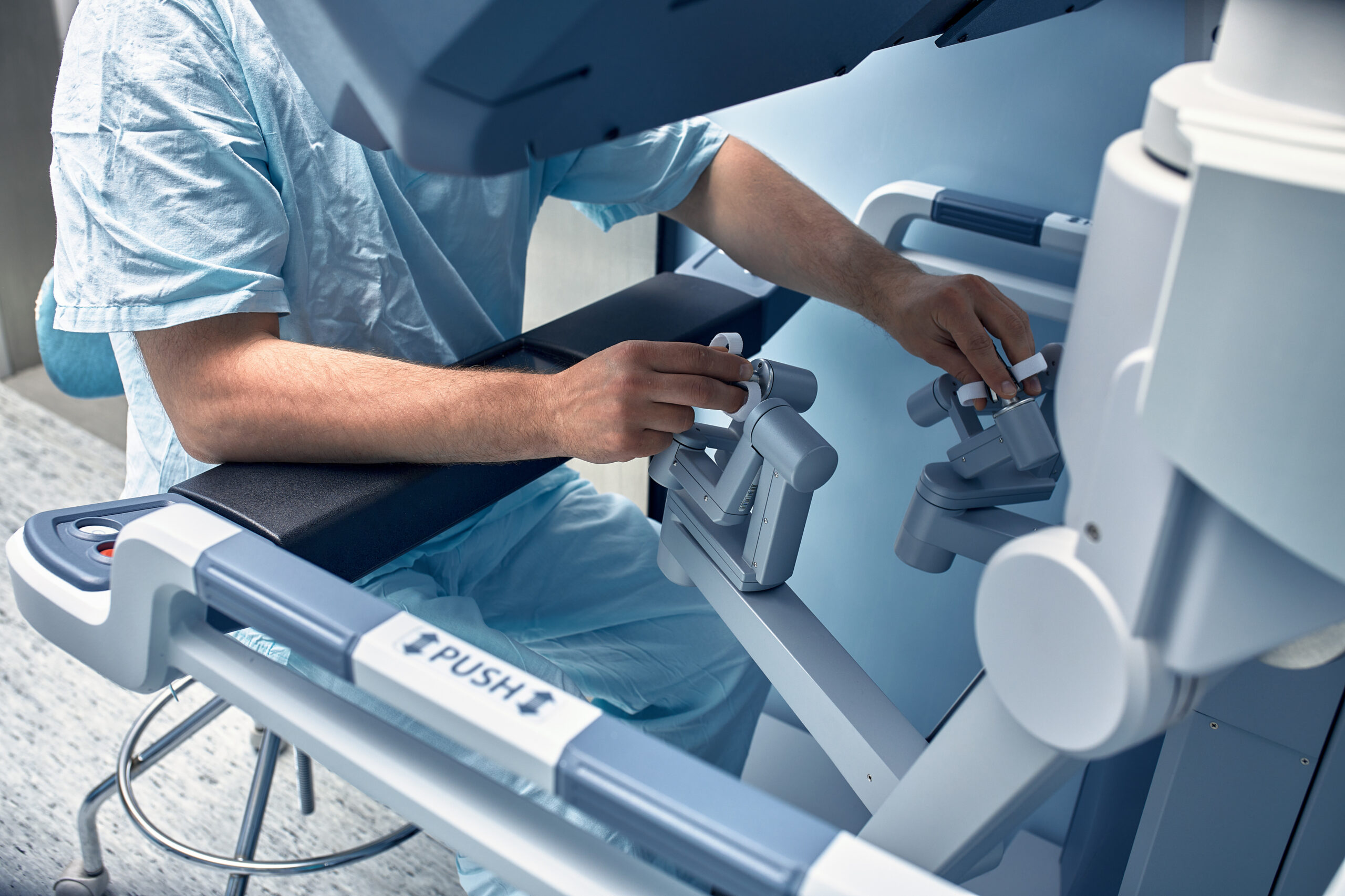
Robotic Surgery
Robotic surgery is an advanced form of minimally invasive surgery where surgeons use robotic systems to perform complex procedures with enhanced precision, flexibility, and control. Through small incisions, surgeons manipulate instruments that are attached to robotic arms, translating their hand movements into smaller, precise actions inside the patient’s body. A high-definition, 3D camera provides a magnified view of the surgical site, allowing for improved visualization. This technology is commonly used in various fields, such as Urology, Gynecology, Cardiothoracic Surgery, and General Surgery. Benefits for patients can include reduced pain and bleeding, shorter recovery times, and less scarring compared to traditional open surgery. Despite its advantages, robotic surgery requires specialized training and carries certain risks, making it crucial for patients to discuss potential benefits and risks with their healthcare provider when considering this surgical option.

Rectal Bleeding
Rectal bleeding refers to the passage of blood through the anus, which may be noticed as blood in or on the stool, in the toilet bowl, or on toilet paper. It can range from subtle streaks of red to significant blood loss and can arise from various causes, including hemorrhoids, anal fissures, diverticulosis, inflammatory bowel disease, or more serious conditions such as colorectal cancer. The color of the blood may help indicate the source of the bleeding: bright red blood typically suggests bleeding from the lower gastrointestinal tract, while darker blood may indicate an upper GI source. Diagnosis often involves a physical examination, medical history, and possibly diagnostic procedures such as a colonoscopy or sigmoidoscopy. Treatment depends on the underlying cause and may include dietary modifications, medications, or, in some cases, surgical intervention. It’s important for individuals experiencing unexplained or persistent rectal bleeding to seek medical evaluation to determine the cause and appropriate treatment.

Anal Cancer
Anal cancer is a relatively rare type of cancer that occurs in the anal canal, which is the opening at the end of the digestive tract where stool exits the body. It primarily arises from the squamous cells lining the anal canal and is often associated with the human papillomavirus (HPV), particularly certain high-risk strains. Symptoms may include rectal bleeding, pain, a lump near the anus, changes in bowel habits, or itching. Diagnosis typically involves a physical examination, imaging studies, and biopsy. Treatment options may include surgery, radiation therapy, and chemotherapy, depending on the cancer’s stage and location. Early detection is crucial for improving outcomes, making awareness of symptoms important for individuals at risk.
Appendicitis
Appendicitis is an inflammation of the appendix, a small, tube-like structure attached to the large intestine. It is considered a medical emergency, often requiring surgical intervention to prevent complications such as perforation and infection. Symptoms typically include abdominal pain that begins near the navel and then shifts to the lower right abdomen, along with nausea, vomiting, loss of appetite, fever, and abdominal swelling. Diagnosis is usually made through a physical examination, imaging tests such as ultrasound or CT scans, and blood tests. Treatment primarily involves an appendectomy, the surgical removal of the appendix, which can often be performed laparoscopically. Prompt treatment is essential to alleviate symptoms and prevent serious complications.
Barrett’s Esophagus
Barrett’s esophagus is a condition in which the normal squamous cell lining of the esophagus is replaced by a different type of cell known as columnar cells, a process called intestinal metaplasia. This change often occurs in individuals with chronic gastroesophageal reflux disease (GERD), where stomach acid frequently irritates the esophagus. Though Barrett’s esophagus itself does not cause symptoms, it is a precursor to esophageal adenocarcinoma, a type of esophageal cancer. Patients may experience symptoms similar to GERD, such as heartburn, difficulty swallowing, and regurgitation. Diagnosis typically involves an upper endoscopy and biopsy to confirm the presence of abnormal cells. Management may include monitoring through regular endoscopies, lifestyle modifications, and medications to control acid reflux, and, in some cases, treatment may be necessary to address dysplasia or cancer risk. Early detection and appropriate management are critical in reducing the risk of progression to esophageal cancer.

Benign Breast Masses
Benign breast masses are non-cancerous growths that can occur in breast tissue, including lumps, cysts, and fibroadenomas. These masses are typically not associated with an increased risk of breast cancer and often do not require treatment unless they cause discomfort or have unusual characteristics. Symptoms may include a palpable lump or swelling in the breast, which may or may not be painful. Diagnosis is made through physical examinations, imaging studies such as mammograms or ultrasounds, and sometimes biopsies to confirm the benign nature of the mass. While benign masses are common, regular monitoring and follow-up with healthcare providers are recommended to ensure that any changes are appropriately evaluated, particularly in women with a history of breast disease. Overall, benign breast masses are usually manageable and do not pose significant health risks.

Breast Cancer
Breast cancer is a type of cancer that originates in the cells of the breast, typically affecting the ducts or lobules. It is one of the most common cancers diagnosed in women, although men can also develop the disease. Risk factors for breast cancer include age, genetic mutations (such as BRCA1 and BRCA2), family history, hormonal factors, and lifestyle factors such as alcohol consumption and obesity. Symptoms may include a noticeable lump or mass in the breast, changes in breast shape or size, dimpling of the skin, or discharge from the nipple. Diagnosis is made through a combination of imaging studies such as mammograms or ultrasounds and a biopsy to confirm the presence of cancer cells. Treatment options vary based on the type and stage of cancer and may include surgery, radiation therapy, chemotherapy, hormone therapy, and targeted therapy. Early detection through regular screenings is crucial for improving outcomes, as it allows for timely intervention and management of the disease.

Culinary Medicine
Culinary medicine is an emerging field that combines the art of cooking with the science of nutrition and medicine to promote health and prevent disease. It focuses on teaching individuals how to prepare healthy, delicious meals while understanding the nutritional value of ingredients and their impact on health. Culinary medicine emphasizes whole foods, balanced diets, and the use of fresh ingredients to enhance wellness and manage specific health conditions, such as diabetes, hypertension, and obesity. This approach encourages hands-on cooking experiences, fostering skills that empower individuals to make informed dietary choices and create healthy meals. By integrating culinary techniques with medical knowledge, culinary medicine aims to bridge the gap between nutritional science and everyday cooking, providing patients and communities with the tools to improve their dietary habits and overall health.
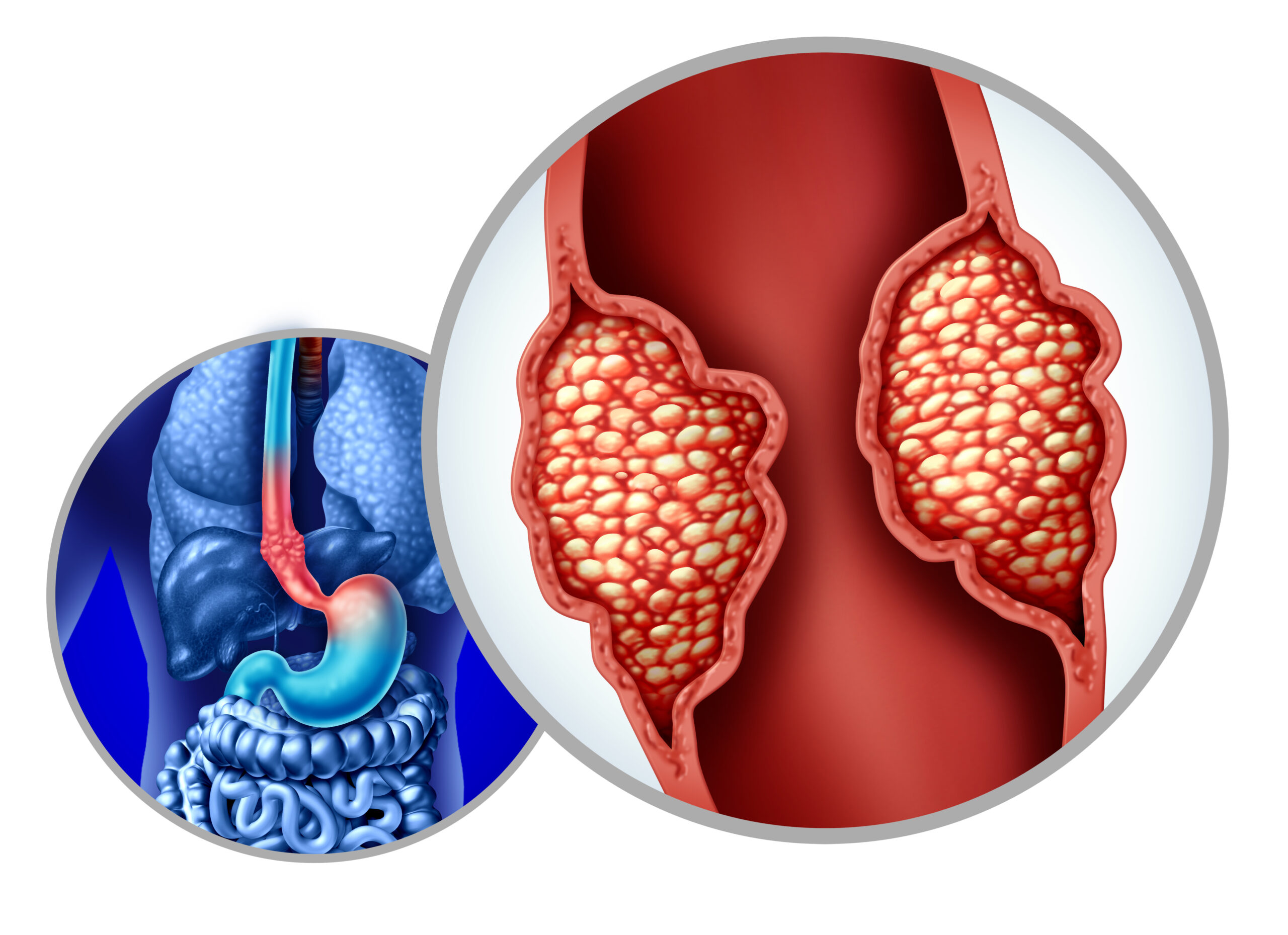
Esophageal Cancer
Esophageal cancer is a type of cancer that originates in the esophagus. It primarily develops from the epithelial cells lining the esophagus and can be categorized into two main types: squamous cell carcinoma and adenocarcinoma. Risk factors for esophageal cancer include chronic gastroesophageal reflux disease (GERD), Barrett’s esophagus, smoking, heavy alcohol consumption, obesity, and a history of certain dietary deficiencies. Common symptoms may include difficulty swallowing (dysphagia), unintended weight loss, chest pain, chronic cough, and indigestion or heartburn. Diagnosis is usually achieved through imaging studies, endoscopy, and biopsy to confirm the presence of cancer cells. Treatment options depend on the cancer stage and may include surgery, radiation therapy, chemotherapy, or targeted therapy. Early detection is vital for improving outcomes, as esophageal cancer can be aggressive and is often diagnosed at an advanced stage.

Hemorrhoids
Hemorrhoids are swollen veins in the lower rectum and anus, similar to varicose veins, and can be either internal or external. Internal hemorrhoids lie inside the rectum and usually present painless bleeding during bowel movements. External hemorrhoids develop under the skin around the anus and can cause itching, swelling, and pain, especially if a blood clot forms. Common causes include straining during bowel movements, chronic constipation or diarrhea, obesity, pregnancy, prolonged sitting, and low fiber diets. Treatment often involves at-home remedies like over-the-counter creams, sitz baths, and increased fiber intake, though severe cases may require medical procedures such as rubber band ligation, sclerotherapy, or surgery to remove the hemorrhoids.

Chronic Nausea
Chronic nausea is a persistent feeling of unease in the stomach that can lead to the urge to vomit, lasting for extended periods or recurring frequently over time. This condition can be indicative of various underlying issues, such as gastrointestinal disorders (like gastritis, peptic ulcers, or irritable bowel syndrome), neurological conditions, metabolic imbalances, or side effects from medications. It may also be associated with psychological factors like anxiety or stress. Identifying the root cause is crucial for effective treatment, which may include dietary modifications, medication to control nausea, addressing any underlying illness, and managing stress. Consulting with a healthcare provider is important for accurate diagnosis and to develop a tailored treatment plan.
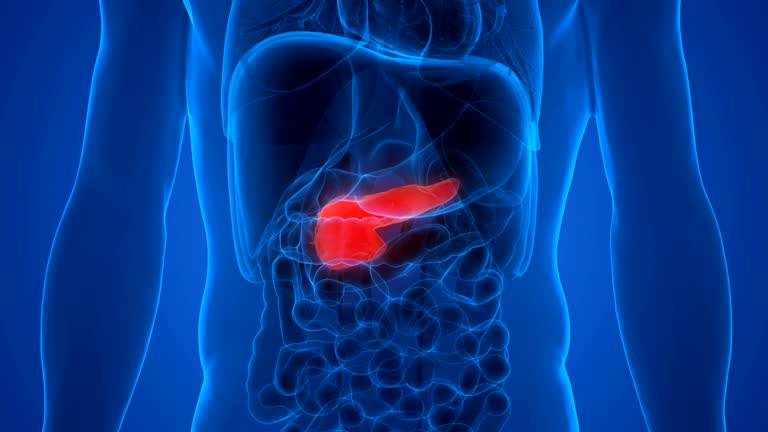
Pancreatic Cancer
Pancreatic cancer is a malignant neoplasm that originates in the tissues of the pancreas, an organ situated behind the stomach that plays a vital role in digestion and blood sugar regulation. This type of cancer is often aggressive and difficult to detect in its early stages due to the deep location of the pancreas and the lack of specific symptoms. As it progresses, symptoms may include jaundice, abdominal or back pain, unexplained weight loss, loss of appetite, and changes in stool. Risk factors include smoking, obesity, chronic pancreatitis, family history of pancreatic cancer, and certain genetic conditions. Treatment options depend on the cancer stage and may include surgery, chemotherapy, radiation therapy, or targeted therapies. Early diagnosis significantly impacts prognosis, so individuals at higher risk may benefit from regular medical checkups and discussing potential screening with their healthcare provider.
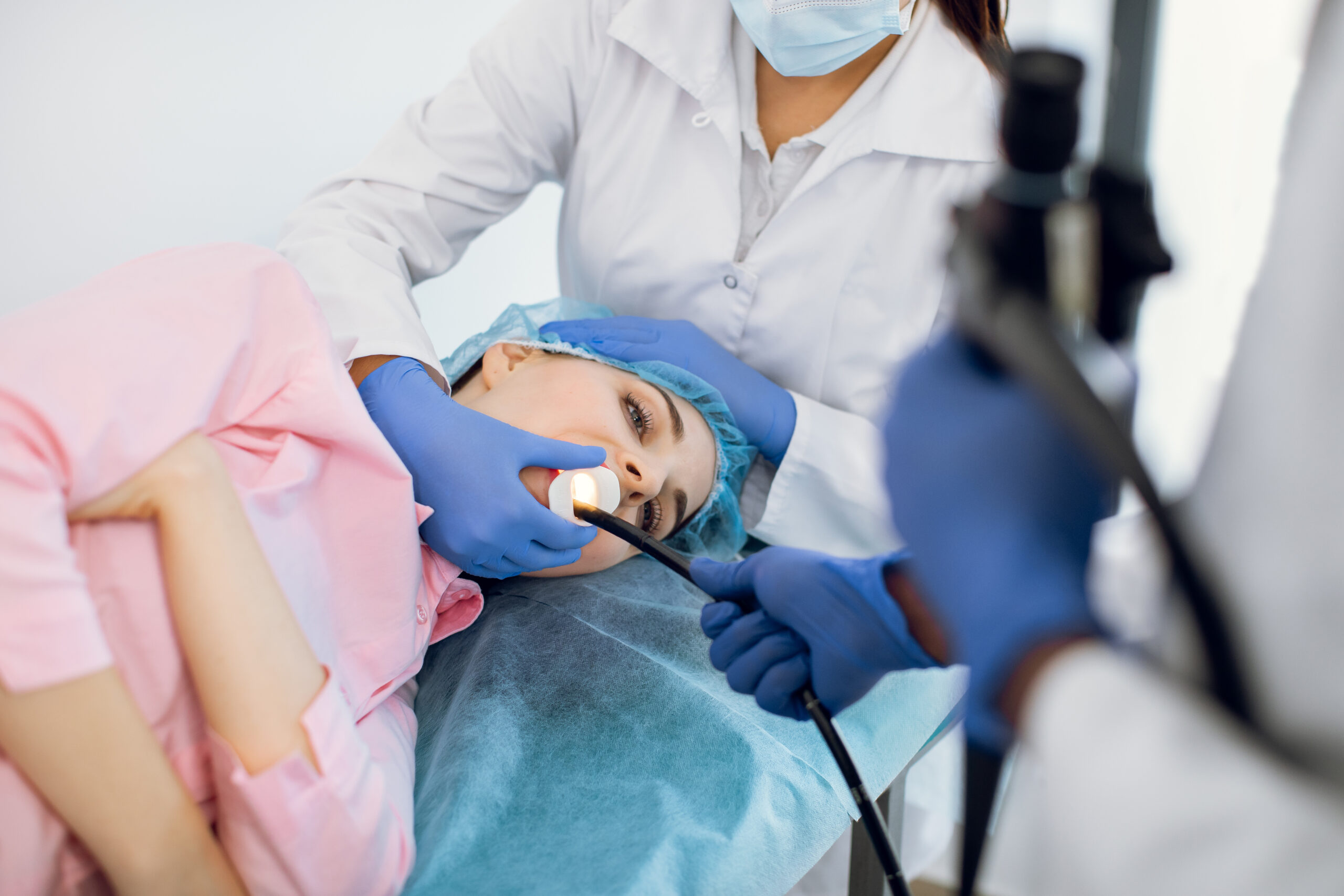
PEG Tube Placement
Percutaneous endoscopic gastrostomy (PEG) tube placement is a medical procedure used to provide direct access to the stomach for nutritional support, usually when oral intake is inadequate or not possible. This is typically indicated for patients with conditions affecting swallowing, such as neurological disorders, cancer, or severe trauma. During the procedure, an endoscope is inserted through the mouth into the stomach, allowing the practitioner to visualize the stomach lining and insert the feeding tube directly through the abdominal wall and into the stomach. This minimally invasive method is generally safe, offering a more durable solution for long-term feeding. Post-placement care includes cleaning the insertion site, monitoring for infection, and managing the tube to ensure proper function and patient comfort. Follow-up with healthcare providers ensures any complications are promptly addressed and nutritional needs are effectively met.
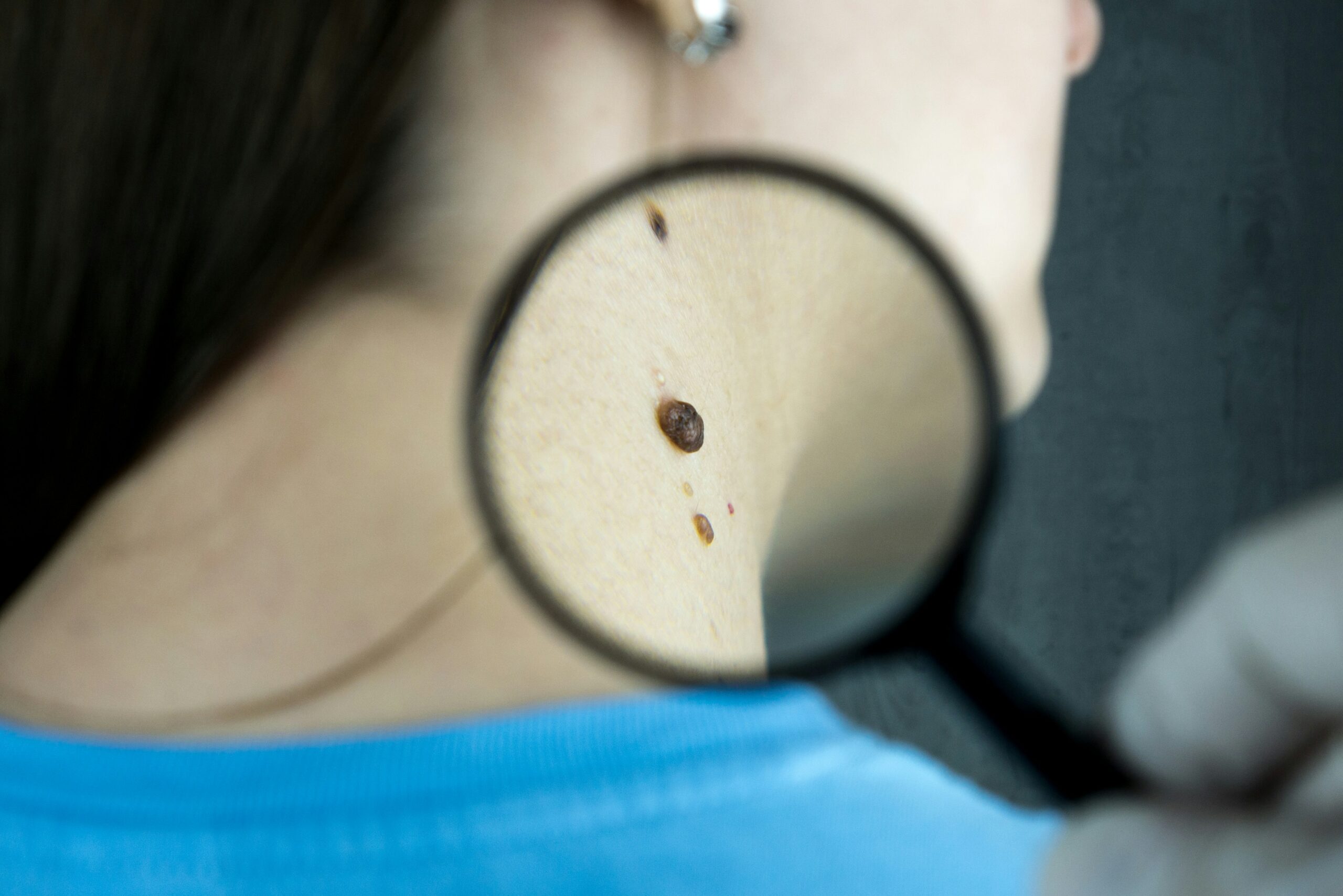
Skin Cancer
Skin cancer is the abnormal growth of skin cells, commonly developing on skin exposed to the sun, but it can also occur in areas not ordinarily exposed. The three main types are basal cell carcinoma, squamous cell carcinoma, and melanoma, each differing in severity and treatment complexity. Basal cell carcinoma is the most common and least aggressive, while melanoma is less common but more serious due to its potential to spread to other parts of the body. Risk factors for skin cancer include excessive UV exposure from the sun or tanning beds, having fair skin, a history of sunburns, excessive moles, and a family history of skin cancer. Symptoms can include new or changing moles, sores that do not heal, and unusual skin growths. Prevention measures include regular use of sunscreen, wearing protective clothing, and avoiding peak sun exposure. Early detection through regular skin checks greatly improves treatment outcomes, making it crucial for individuals to monitor their skin and consult a healthcare provider if they notice any changes.
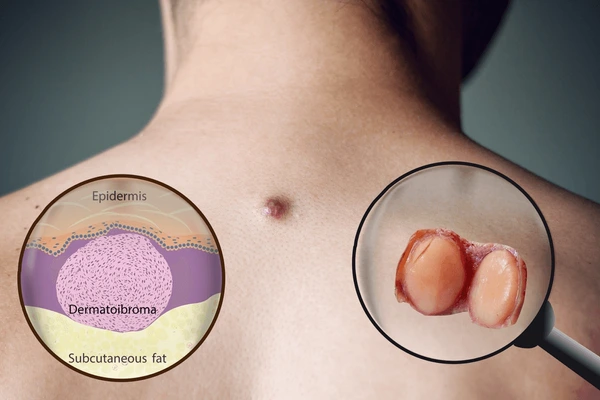
Soft Tissue Tumors
Soft tissue masses refer to abnormal lumps or growths that develop in the body’s soft tissues, which include muscles, fat, nerves, tendons, and blood vessels. These masses can be benign (non-cancerous) or malignant (cancerous), with lipomas being common benign examples, while sarcomas represent malignant possibilities. The cause of these masses varies, including genetic factors, injuries, or no identifiable cause. Symptoms or characteristics can include a noticeable lump, which may be painless or painful, and changes in size over time. Diagnosis typically involves a physical examination, imaging studies such as ultrasound or MRI, and sometimes a biopsy to determine the nature of the mass. Treatment depends on whether the mass is benign or malignant and may range from simple observation to surgical removal, and in the case of malignancy, could include additional treatments like radiation or chemotherapy. Prompt evaluation by a healthcare professional is recommended for any new or changing soft tissue masses to ensure appropriate management.

Stomach Cancer
Stomach cancer, also known as gastric cancer, occurs when malignant cells form in the lining of the stomach. It often develops slowly over many years and may go undetected in its early stages due to a lack of specific symptoms. As the cancer progresses, symptoms can include persistent indigestion, stomach pain, nausea, loss of appetite, weight loss, and, in more advanced cases, vomiting blood or having black, tarry stools. Risk factors include infection with Helicobacter pylori bacteria, smoking, a diet high in salty and smoked foods, a family history of stomach cancer, and certain genetic conditions. Diagnosis usually involves a combination of endoscopy, imaging tests, and biopsy to confirm the presence of cancerous cells. Treatment options may include surgery, chemotherapy, radiation therapy, or targeted therapy, depending on the cancer’s stage and location. Early detection is critical to improving outcomes, so individuals experiencing persistent gastrointestinal symptoms should seek medical evaluation.
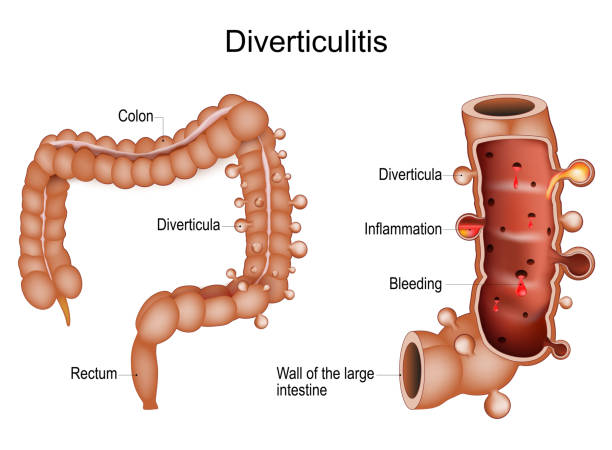
Diverticulosis and Diverticulitis
Diverticulosis and diverticulitis are related conditions involving the colon. Diverticulosis is the formation of small pouches, or diverticula, in the wall of the colon, which generally don’t cause symptoms and might only be discovered during routine screenings or tests for other issues. The exact cause is unclear, but it is associated with a low-fiber diet and aging. Diverticulitis occurs when these pouches become inflamed or infected, leading to symptoms such as abdominal pain, particularly in the lower left side, fever, nausea, and changes in bowel habits. Treatment for diverticulitis may involve antibiotics, a liquid diet to allow the colon to heal, and in more severe or recurrent cases, surgery might be required. Increasing dietary fiber can help manage diverticulosis and reduce the risk of diverticulitis. Regular medical follow-up is important to manage both conditions effectively.
